The research at the USC Michelson Center for Convergent Bioscience includes collaborators from USC Keck and Stanford.
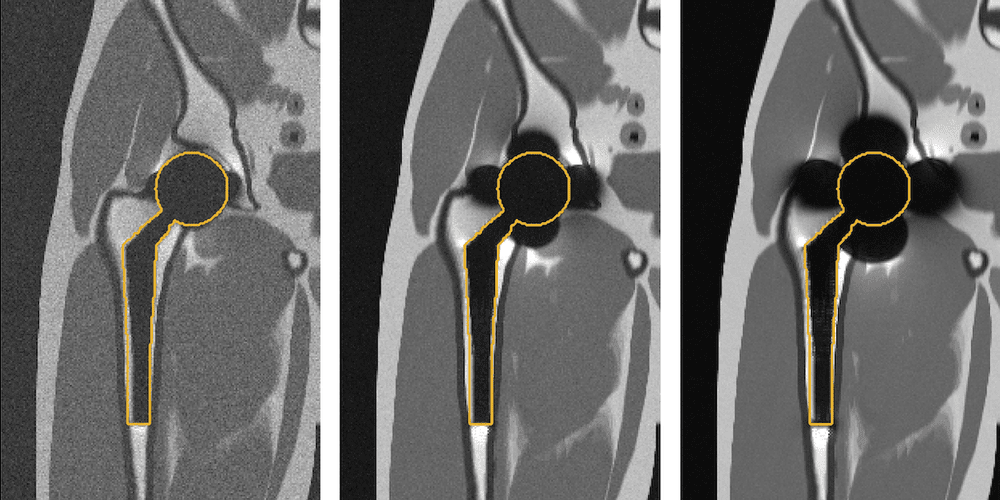
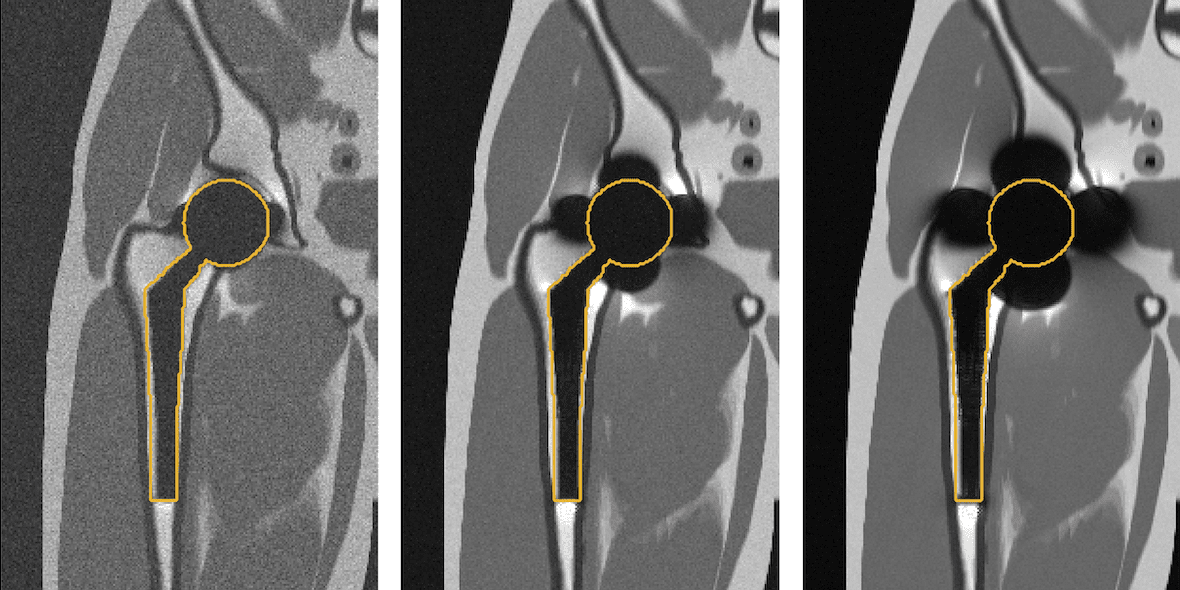
Simulated imaging of a total hip replacement using (left to right) 0.55 Tesla, 1.5 Tesla, and 3 Tesla MRI. Notice the reduced distortions at lower field strengths. (Photo credit: Kübra Keskin)
By Ben Paul
As implant technology improves and the American population continues to age, the number of people living with implants has grown. In fact, today 32 million people in this country are living with a medical implant. That’s nearly 10 percent of the population. While these devices have certainly improved the lives of many people, challenges remain. One of the biggest of these challenges is revision surgery. As implants break down or the body struggles to accept the foreign object, doctors often must go back into a patient to update, remove, or replace devices – a costly and sometimes dangerous process.
Could we one day see a world where implants last forever, and never need to be updated or replaced? A new 5-year NIH-funded grant led by USC Viterbi aims to solve that problem.
The first hero in this story is a new tool housed at USC Viterbi’s Michelson Center for Convergent Bioscience: an ultra-rare low-field MRI machine that is one of only three of its kind in the world. “This machine has capabilities unlike MRIs you’ll find in hospitals,” said Krishna Nayak, Professor of Electrical and Computer Engineering, Biomedical Engineering, and Radiology and lead PI on the grant. “Soft tissues near metallic implants are where a lot of the problems arise, specifically within 1-2 millimeters of the implant surface. While imaging that tissue is nearly impossible with traditional MRIs, ours can capture images of this space.”
This machine, which came online in 2021, is already hard at work. In addition to imaging around implants, the researchers are also using it for improved fetal imaging, improved lung imaging, and improved cardiac perfusion imaging – three other important areas that traditional MRIs aren’t as good at.
The second hero of the story is the diverse and collaborative background of the researchers. The grant brings together engineers from USC Viterbi and Stanford and radiologists and orthopedic surgeons from USC Keck School of Medicine. The diversity of perspectives among the researchers is one of the team’s biggest strengths and allows them to approach these challenges from several different perspectives at once; engineers specializing in metal implant imaging and the physics of low-field MRI work to develop improved imaging outcomes. Meanwhile, orthopedic surgeons and radiologists help inform how the new technologies can best be utilized in the real world for the patient.
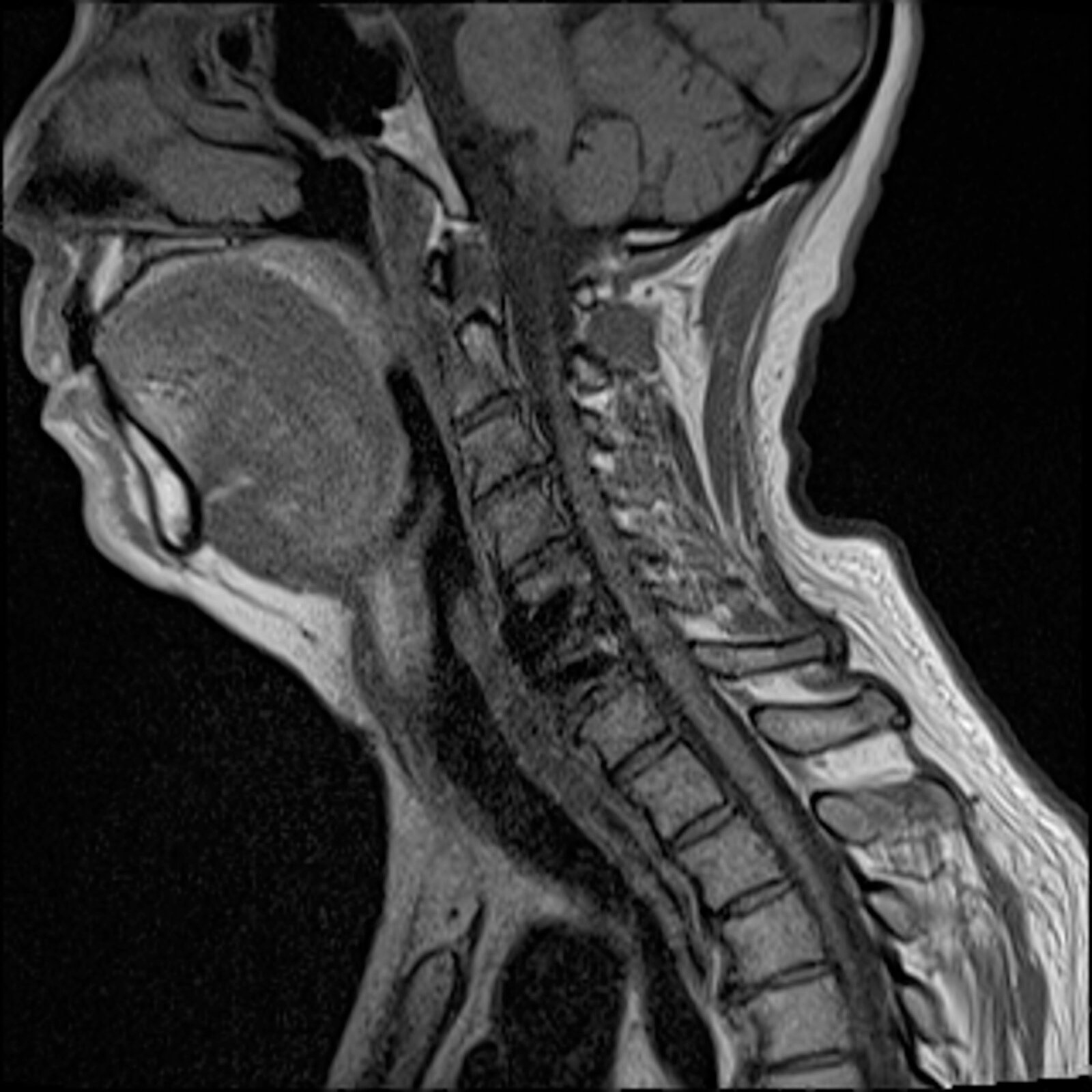
Image of a volunteer with an implant at cervical spine, imaged using novel 0.55 Tesla MRI (Photo credit: Kübra Keskin)
Jay Acharya, associate chief of neuroradiology, assistant professor of clinical radiology, director of spine imaging and intervention at Keck School of Medicine of USC, and co-PI is excited about the project. “I see images of patients with spinal implants daily. One of our biggest challenges is being able to see clearly what might be going wrong with a device implanted in such a sensitive area. With this new technology, we hope to assess the tissue immediately surrounding the metallic implant, which can provide insight into whether the hardware is failing.”
I hope that through this research we can provide real solutions that will have an immediate impact on the health and happiness of our patients,” he said.
The team is already scanning patients in the Dynamic Imaging Science Center (DISC) where the MRI machine is housed. They plan to eventually capture data from 140 patients. The long-term goal of the study is to better understand when implants are failing to help manufacturers optimize new devices and help doctors avoid unnecessary surgeries. “With this large data set, we will test our theory that low-field MRIs can and should be used for better imaging in clinical settings in the future,” said Nayak.
This article was originally published by USC Viterbi.